By Michelle Place CRNP-PC
Pain in your ear is a pain in my…
Your child has been up for the majority of the night crying and either saying that his ear hurts or indicating this is true by tugging and pulling at his ears. As soon as your pediatrician’s office opens you call for an appointment, secretly (or not so secretly) hoping that the doctor will find an ear infection because at least you will get medicine to offer your child some relief.
Unfortunately, young children often have a difficult time localizing ear pain. Complaints of pain in the ear can be caused by the eruption of new molars, sore throat, viral swelling or, our sworn enemy, the common cold. In addition, the number one reason that infants pull at their ears is that they have discovered that they are there.
If it is found that the pain is the result of an ear infection, it is important to realize that antibiotics do not provide symptomatic relief during the first 24 hours. In fact, 30% of children younger than 2 years will still have pain, fever or both even after 3-7 days of treatment.
In contrast, analgesics do relieve pain associated with ear infections or acute otitis media (AOM) and should be used whether antibiotic therapy is prescribed or not. They should be continued as long as they are needed. Ibuprofen is very effective in treating ear pain, acetaminophen can also be used. These oral pain relievers are your best bet because there is limited evidence that ear drops are effective in providing relief.
An Otoscope of My Very Own
Many times parents say that they wish they had “one of those ear things” at home so they could look at their children’s ears and decide if they need treatment without bringing them to the doctor’s office. The truth is making the diagnosis of ear infection is sometimes very difficult even after years of training and experience looking at ear drums all day long. Here is what the ear drum should look like:
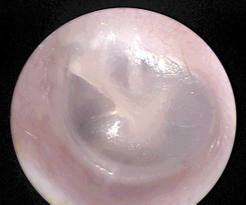
Here are some ear drums that are not “normal” but one of them does not require immediate treatment with antibiotics. Can you tell which is which?
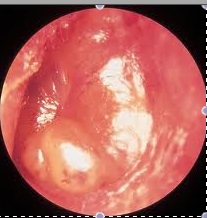
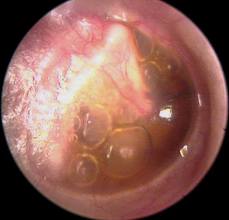
There is no gold standard for the diagnosis of an ear infection like a positive throat culture means you have strep throat. In fact, AOM has a spectrum of signs as the disease develops so it’s appearance changes over time. According to the new guidelines, moderate to severe bulging of the tympanic membrane or eardrum is the most important characteristic needed to diagnose an ear infection. That means the ear on the left would score the drugs while the one on the right is caused by the presence of fluid and would not benefit from treatment.
Antibiotics or No Antibiotics, That is the Question
Antibiotics should be prescribed immediately to those children with moderate to severe bulging of the ear drum accompanied by severe ear pain, ear pain that has lasted for at least 48 hours, fever of 102.2 or higher, drainage from the ear (not related to swimmer’s ear), and children aged 6-23 months especially if they have infections in both ears. For everyone else it is safe to hold off on treatment because most cases spontaneously resolve without complications.
Antibiotics come with many unwanted side effects. They can cause a rash all over which may or may not be an allergy. Diarrhea and it’s resultant diaper rash are another common outcome. The overuse of these medications has produced bacteria that is resistant to many antibiotics. The result of these superbugs is a loss of efficacy in the medicines when we really need them.
Watchful Waiting
If the decision is made to hold off on antibiotics it does not mean sitting back and doing nothing. Ibuprofen should be given for fever and discomfort. You need to watch your child carefully. If symptoms worsen or there is no improvement within 72 hours then they should be seen again. Antibiotics will be given if your child fails observation.
I Want the Strong Antibiotic
When it is determined that your child will benefit from an antibiotic, it is important to choose the one that has the highest probability of being effective against the bug most likely causing your child’s ear infection. Studies show that unless your child has received it within the last 30 days, Amoxicillin is the drug of choice to treat ears, which we carry right here in our office in our InstyMeds machine. Often parents say that they want something ”stronger” or that amoxicillin “does not work for their child” but it is not the person against whom the drug works but the bacteria causing the infection.
When your child is placed on antibiotics you may find the symptoms worsen slightly in the first 24 hours but should start to improve after that. If there is no improvement seen after 72 hours there might be a benefit from changing the antibiotic. A lack of improvement may also be due to the fact that ear infections are usually accompanied by viral infections whose symptoms are immune to antibiotics, therefore, a change in antibiotic may not be required in some children with mild persistent symptoms.
Back to Back to Back Ear Infections
Sometimes it seems that the ear infection never stops. As soon as one bout of antibiotics is finished another needs to be started. Recurrent ear infections are defined as the occurrence of 3 or more episodes of AOM in a 6-month period OR 4 episodes in the past year with at least 1 having been diagnosed in the preceding 6 months. If your child meets this criteria they may be a candidate to have tubes placed that will keep the ears well drained. To keep an accurate record it is important that your child be evaluated in one medical home. An ear infection is not an emergency. It is important that you be seen as much as possible by your regular doctor rather than at an Urgent Care Clinic or the ER.
A Good Defense is the Best Offense:
- PCV7 vaccine was introduced in 2000 as part of the routine vaccine schedule. It provides immunity against 7 strains of the bacteria which is most often the cause of ear infections. Since that time medical office visits for otitis were reduced by up to 40%. In 2010 it was changed to PCV13, so now we give protection against, you guessed it, 13 strains..
- Get your flu shot! Many studies have demonstrated 30-55% efficacy of influenza vaccine in prevention of ear infections during the respiratory illness season. Check out our available WALK-IN Flu Clinic dates to get the whole family vaccinated.
- Multiple studies provide evidence that breastfeeding for at least 4 months reduces episodes of ear infections. There seems to be a dose response with some protection from partial breastfeeding and the greatest protection from exclusive breastfeeding for 4-6 months. If you’ve been struggling with breastfeeding, email our lactation consultant at lactation@potomacpediatrics.com.
- Your baby’s health is the perfect reason to quit! Eliminating exposure to passive tobacco smoke probably will reduce the incidence of AOM in infancy.
- Avoiding bottle propping and eliminating pacifier use in the second 6 months of life may reduce AOM incidence.
When to call the doctor if your child complains of ear pain and you are worried about an ear infection:
- severe ear pain
- ear pain that has lasted for at least 48 hrs
- fever of 102.2 degrees or higher
- drainage (pus or blood) coming from the ear
An ear-check appointment is quick and easy at Potomac Pediatrics. Call us for a same-day appointment at (301) 279-6750 or contact us and speak to one of our advice nurses.
![]()






